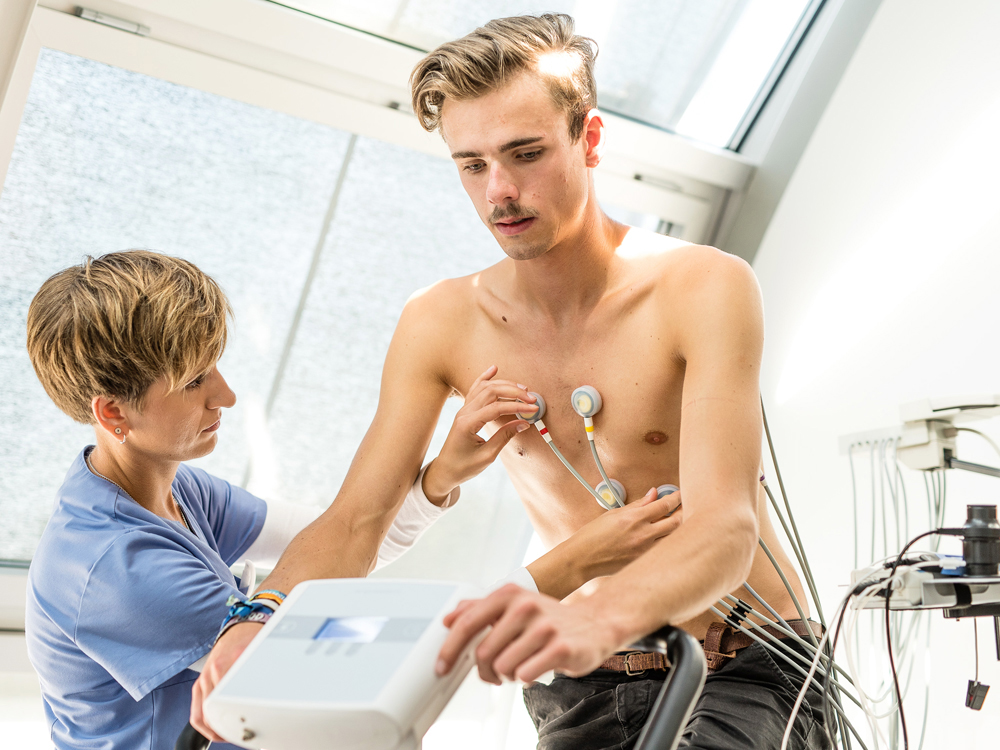
Cardiology
Heart and vascular diseases are known as endemic diseases. These will be handled by a cardiologist. At Klinikum Stephansplatz in Hamburg, cardiology patients benefit from close interdisciplinary collaboration between cardiology, endocrinology, pulmonology, neurology and rheumatology.
What services can patients expect from cardiologists at MEDIZINICUM Hamburg (Klinikum Stephansplatz)? Of course, a cardiological check-up exam with comprehensive evaluation of the current state of the cardiovascular system. All non-invasive examination options are available for this purpose. In addition, the risk of myocardial infarction can be determined and, where appropriate, preventive measures discussed and taken.